Natural cartilage lubricant and cushion hyaluronic acid may reduce joint pain.
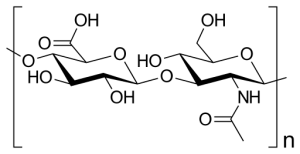
Hyaluronic acid is a naturally present compound in and around joints. It has been shown to provide such potential uses in joint health as:
- Managing inflammation. Hyaluronic acid helps in both initiating early inflammation for recovery and stopping the natural inflammatory response from going overboard.
- Fortifying cartilage. Hyaluronic acid serves as a lubricant and cushion for cartilage while also minimizing its breakdown.
Overview
One of the principal components of the extracellular matrix, hyaluronic acid is a type of glycosaminoglycan that is naturally present in the human body. An average person carries approximately 15 grams of pure hyaluronic acid at all times, with one-third of it being broken down and remade every day. The highest concentrations of hyaluronic acid are found in the fluid of the eyes and joints.
Since the 1970s, hyaluronic acid has been highly regarded as an accompanying therapeutic for eye surgeries, skin conditions, wound healing, and articular disorders. Its beneficial use in joint health has been well documented in animal studies, and many proponents of natural supplementation support its use by humans.
As an important part of articular cartilage and synovial fluid, as well as a role player in cell growth, medical professionals concur that hyaluronic acid is an essential part of healthy joints. The extent to which hyaluronic acid supplements further promote joint health continues to be investigated today. It remains one of the most commonly used joint health ingredients.1
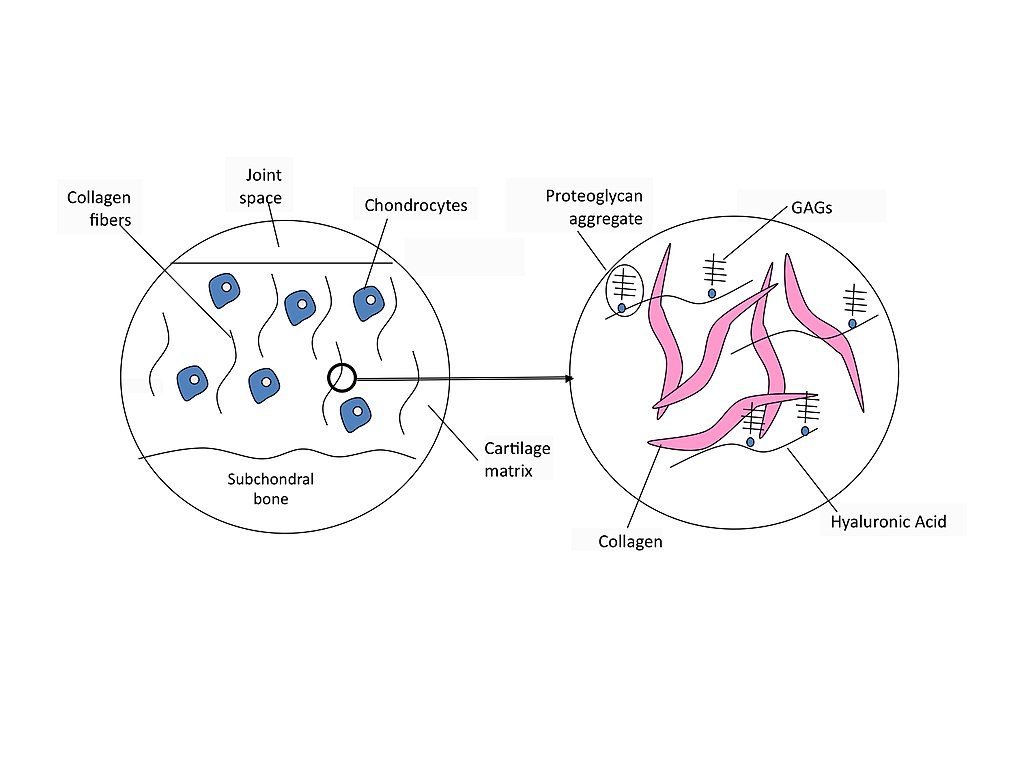
How Hyaluronic Acid Might Help With Joint Health
Managing inflammation
Hyaluronic acid initiates the inflammatory process during wound healing but also limits the amount of inflammation that can take place via a negative feedback loop.2 This may help curb pain and swelling in joint recovery.
Lubricating and cushioning cartilage
Hyaluronic acid is present as a coat around cartilage cells and is believed to act as a lubricant and cushion to enhance the sliding between adjacent tissue layers.3 In addition, hyaluronic acid is known to bind to proteins and form a compound known as HAPLN1 that absorbs water and increases the resilience of cartilage, i.e., its resistance to compression.
Preventing cartilage breakdown
Hyaluronic acid may be capable of restricting the breakdown of cartilage in joint.4 It has specifically been shown to diminish cartilage breakdown in osteoarthritis by inhibiting 3 processes: 5 6
- Inhibiting the release of enzymes that are responsible for deteriorating cartilage
- Reducing the presence of chemicals that promote cell breakdown
- Stopping phagocytes from “eating” cartilage cells
Hyaluronic Acid Benefits & Uses for Joint Health
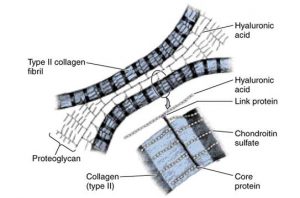
As a fundamental component of joint fluid and cartilage, hyaluronic acid is vital to joint health. Hyaluronic acid supplements may thus impart a number of benefits, though the true extent of their impact is hotly debated: 7
- Relieving joint pain8
- Diminishing joint stiffness
- Decreasing progressive joint damage
- Improving joint function
Similar to other joint supplements, such as MSM and glucosamine, hyaluronic acid supplements have also been used to help manage clinical joint conditions, particularly osteoarthritis, with varied success. Some medical factions go so far as to claim that hyaluronic acid is a legitimate treatment for osteoarthritis.9 Further clinical research is certainly warranted.
Research
Human Research
Hundreds of clinical studies have examined the potential benefits of hyaluronic acid for joint health, with a focus on alleviating joint pain and stiffness, as well as improving function. The results are somewhat conflicting, though they generally present a favorable outlook on hyaluronic acid as a remedy for joint conditions. A detailed selection of the research follows.
In this randomized, double-blind, placebo-controlled investigation, 20 adults with knee osteoarthritis were given either a placebo or 80 mg of 60% hyaluronic acid extract from chicken combs every day for 8 weeks. The hyaluronic acid group experienced statistically significant improvements in pain, stiffness, and physical function compared to baseline, but only slightly higher, non-statistically significant improvements compared to placebo.
- The researchers concluded that “daily supplementation with oral hyaluronic acid from a natural extract of chicken combs (Hyal-Joint) was useful to enhance several markers of quality of life in adults with osteoarthritis of the knee.”10
In this randomized investigation, 60 patients with knee osteoarthritis were given either a transcutaneous electrical nerve stimulation (TENS) or an injection of hyaluronic acid known as Hylan G-F 20 directly into the knee joint once a week for 3 weeks. Pain and stiffness decreased in both groups. Neither treatment significantly affected physical function.
- The researchers concluded that “these therapies used in combination may alleviate symptoms in patients with OA.”11
Hyaluronic acid as Suplasyn® (60 mg/wk) may reduce joint pain
In this non-controlled, open-label investigation, 537 patients with osteoarthritis of the knee were given intra-articular injections containing 20 mg of hyaluronic acid as Suplasyn® 3 times a week for 3 weeks. Hyaluronic acid injections led to significant decreases in pain. Very few adverse side effects were reported apart from local pain and swelling.
- The researchers concluded that “intraarticular hyaluronic acid injections were highly effective in improving resting and walking pain in patients with osteoarthritis of the knee.”12
In this randomized, double-blind, placebo-controlled investigation, 120 patients with knee osteoarthritis were given a placebo, anti-inflammatory drugs with placebo, anti-inflammatory drugs with 20 mg of hyaluronate sodium, or placebo with hyaluronate sodium once a week for 3 weeks. Hyaluronic acid was found to be as effective as anti-inflammatory drugs at relieving knee pain while resting and significantly better during physical activity.
- The researchers concluded that “for resting pain relief, hyaluronate sodium seems to be as effective as NSAIDs. Further, for pain with physical activity and functional performance, hyaluronate sodium may be superior to placebo alone or NSAIDs alone.”13
Hyaluronic acid as Hyalgan (20 mg/wk) may relieve pain more than anti-inflammatory medication
In this randomized, double-blind, masked observer, placebo-controlled investigation, 495 patients with osteoarthritis were given a placebo, anti-inflammatory medication, or a 20 mg injection of hyaluronic acid as Hyalgan once a week for 5 weeks. Compared to the placebo, the hyaluronic acid group had more improvements in pain relief when walking. Pain relief was marked at 47.6% with hyaluronic acid, 36.9% with the medication, and 33.1% with the placebo.
- The researchers concluded that “IA injections of HA (Hyalgan) in patients with OA of the knee are generally well tolerated, provide sustained relief of pain and improved patient function.”14
In this randomized, double-blind, placebo-controlled study, 588 patients with chronic knee osteoarthritis were given either a saline placebo or 20 mg of a hyaluronic acid injection known as Euflexxa (IA-BioHA) once a week for 3 weeks. Pain reduction was 53% for the hyaluronic acid group compared to 38% for the placebo group. Hyaluronic acid also led to significant improvements in health-related quality of life (HRQoL) and knee function.
- The researchers concluded that “IA-BioHA therapy resulted in significant OA knee pain relief … [and] significant improvements in joint function, treatment satisfaction, and HRQoL.”15
Hyaluronic acid might not reduce joint pain or improve function significantly more than placebo
In this review of 22 trials, elderly patients with osteoarthritis of the knee experienced slight pain reduction after taking hyaluronic acid, but not to a statistically significant degree. No notable improvements in knee function were found. There was also a slightly higher chance of adverse side effects occurring in the hyaluronic acid group.
- The researchers concluded that “intra-articular hyaluronic acid has not been proven clinically effective and may be associated with a greater risk of adverse events.”16
In this randomized, non-controlled investigation, 160 patients with knee osteoarthritis were given either 20 mg of hyaluronic acid (HA) 3 times at 1 week intervals or a platelet-rich plasma (PRP) 3 times at 4 week intervals. Joint pain significantly improved in both groups compared to baseline, but PRP produced better results than HA.
- The researchers concluded that “PRP injection is more efficacious than HA injection in reducing symptoms and improving quality of life and is a therapeutic option in select patients with knee OA who have not responded to conventional treatment.”17
Hyaluronic acid as XLHA (60 mg) may be a safe and effective treatment for osteoarthritis
In this randomized, double-blind investigation, 287 patients with osteoarthritis were given a placebo, a cross-linked hyaluronate injection (XLHA), or a linear high molecular hyaluronate control injection (HMWHA). Hyaluronic acid in the form of XLHA proved to be just as effective as HMWHA at relieving joint pain.
- The researchers concluded that “XLHA was non-inferior to three weekly injections of HMWHA in terms of WBP reduction, and supports XLHA as an effective and safe treatment for knee osteoarthritis.”18
Hyaluronic acid as Durolane® may be a viable pain relief treatment for osteoarthritis
In this randomized investigation, 54 patients with knee osteoarthritis were given injections of 1 of 2 types of hyaluronic acid injections: NASHA as Durolane® or HA as Go-ON®. The NASHA group experienced a statistically significant improvement in pain relief compared to the HA group.
- The researchers concluded that “our study supports the use of the NASHA class of products in the treatment of knee OA.”19
Dosage for Joints
- Successful clinical research studies use from 80 mg of hyaluronic acid capsules per day, or 20 – 60 mg of hyaluronic acid injections per week.
- Typical hyaluronic acid supplements range from 100 – 300 mg per day.
Available Forms
- Intra-articular injection
- Capsules or pills
- Fluid or drink
- Powder
Supplements in Review Says
- Hyaluronic acid 100 mg for joint health.
Hyaluronic acid may reduce joint pain due to osteoarthritis. As a fundamental component of joints, hyaluronic acid is a vital contributor to joint health. Supplementation with it has been shown to reduce joint pain, stiffness, and swelling, as well as improve function. Its safety and effectiveness are still being scrutinized.
Start with 100 mg of hyaluronic acid capsules. Hyaluronic acid seems most effective as an intra-articular injection, but we suggest starting with capsules for supplementary use.
Leave a Reply