Vitamin D supplementation can boost immune function in individuals with suboptimal levels.
- Support immune function. Low vitamin D levels are associated with increased risk of colds, flu, allergies, autoimmune disorders, and other illnesses.
Overview
Popularly known as the “sunshine vitamin” because its synthesis is promoted by exposing the skin to sunlight, vitamin D is an essential nutrient involved in bone health, muscle function, testosterone production, and other processes.
In recent decades researchers have discovered that vitamin D also plays an important role in immune function. As one highly-cited review paper summarizes, “vitamin D emerges as a promising and relatively safe nutrient for new strategies in the prevention and adjunctive treatment of diseases caused by impaired immune-homeostasis.”1
Indeed, current research findings demonstrate that individuals deficient in vitamin D can expect to see significant immunity benefits from supplementation. And according to one recent study, vitamin D deficiency may affect as many as 42% of American adults, being particularly common in African-Americans (82%) and Hispanics (69%).2 These statistics help explain the growing popularity of vitamin D supplements, especially during the winter when we get less sun exposure.

How Vitamin D Might Help With Immunity
Supporting optimal immune function
Vitamin D appears to have a wide array of functions in the immune system such as preventing excessive production of inflammatory cytokines and promoting the production of anti-microbial compounds.3 Research shows that immune cells have vitamin D receptors and produce enzymes that use vitamin D and convert it into its active form calcitriol. As such, vitamin D appears to be required for healthy immune system function, similar to zinc and vitamin C.
Vitamin D Uses & Benefits for Immunity
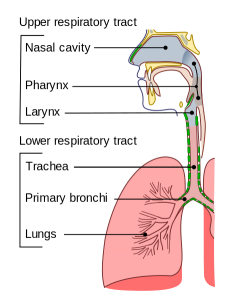
Although more trials looking at the link between vitamin D supplementation and specific illnesses are needed, existing research evidence backs its immunity benefits. In addition, there is a large amount of data showing that low vitamin D and calcitriol levels are associated with respiratory tract infections such as cold and flu, inflammatory conditions such as allergies, asthma, and IBD, autoimmune disorders, and other conditions.4 5 6
Nonetheless, it’s important to reiterate that vitamin D supplementation is unlikely to have much affect in the absence of deficiency.
Research
Human Research
Studies of vitamin D suggest that it’s deficiency can make you more susceptible to a wide range of illnesses.
Lower vitamin D levels are associated with respiratory infections
This Finnish study explored the link between vitamin D levels and acute respiratory infections. Eight hundred young men had their vitamin D levels measured and were followed up for 6 months to see how many days they were sick due to respiratory infections. The major finding of the study was that men with vitamin D levels lower than 40 nmol/L missed more days due to respiratory infection.
- The researchers concluded that “Clinical trials of vitamin D supplementation are needed to investigate whether it enhances immunity to microbial infections.”7
Low vitamin D seems to increase respiratory infection risk in athletes
This study looked at the effects of vitamin D status on immunity in endurance athletes. Two hundred and twenty-five athletes had their blood tested over a 16-week training period during the winter.
The study found that athletes with deficient vitamin D were far more likely to get upper respiratory tract infections (URTI), and also had more severe and longer-lasting symptoms. In addition, they also had lower levels of certain immunity markers, such as cytokine production.
- The researchers concluded that “Low vitamin D status could be an important determinant of URTI risk in endurance athletes and mucosal as well as systemic immunity may be modified via vitamin D-dependent mechanisms.“8
Vitamin D may help with atopic dermatitis
This study tested the efficacy of vitamin D for helping children with atopic dermatitis (AD), a condition that involves skin inflammation. Thirty-nine children with AD were supplemented with vitamin D for three months, resulting in a reduction of elevated cytokine levels (IL-2, IL-4, IL-6, IFN-γ, TNF-α) and a reduction of AD severity.
- The researchers concluded that “This study showed vitamin D supplementation to be an effective treatment in reducing AD severity in children…“9
Vitamin D (200 – 4000 IU) may boost immunity during winter time
This randomized, double-blind, placebo-controlled study examined the effects of vitamin D supplementation on immunity and skeletal muscle function. Thirty young adults with normal vitamin D levels were given placebo or vitamin D (200 or 4000 IU) daily for 28 days in the winter. The study found that both the low and high doses prevented the winter-associated drop in IL-5, a cytokine molecule involved in protection against infections.
- The researchers concluded that “…a low-daily dose of supplemental vitamin D prevents serum 25(OH)D and IL-5 concentration decreases…Considering that IL-5 protects against viruses and bacterial infections, these findings could have a broad physiological importance regarding the ability of vitamin D sufficiency to mediate the immune systems protection against infection.”10
Vitamin D supplementation does not reduce respiratory infection risk in non-deficient adults
This randomized, double-blind, placebo-controlled study examined whether vitamin D supplementation would reduce the severity and risk of upper respiratory tract infections (URTIs) in adults with healthy vitamin D levels. Three hundred and twenty-two adults were given placebo or 200,000 IU vitamin D3 followed by 100,000 IU monthly.
Although supplementation resulted in a further increase of vitamin D levels, there was no significant difference between placebo and vitamin D groups in the number of URTIs per person, number of days sick with URTIs, or duration/severity of symptoms.
- The researchers concluded that “monthly administration of 100,000 IU of vitamin D did not reduce the incidence or severity of URTIs in healthy adults.”11
Vitamin D (2000 IU) may improve autoimmune conditions
This randomized, placebo-controlled study explored the link between vitamin D and systemic lupus erythematosus (SLE), a chronic autoimmune condition. Two hundred and sixty-seven patients with SLE were given placebo or vitamin D3 (cholecalciferol) 2000 IU daily for 12 months.
The study found that 69% of the participants had low and 39% had deficient vitamin D levels, and that vitamin D supplementation significantly improved the disorder.
- The researchers concluded that “Vitamin D supplementation in patients with SLE is recommended because increased vitamin D levels seem to ameliorate inflammatory and hemostatic markers and show a tendency toward subsequent clinical improvement.“12
Dosage for Immunity
- Research studies have used doses ranging from as low as 200 to as high as 4000 IU vitamin D daily
- Most vitamin D supplements provide 1000 – 5000 IU doses
- The most common form of vitamin D in the diet and supplements is D3 (cholecalciferol)
- Early research indicates that vitamin D3 may be better than D2 at sustaining vitamin D levels13
Supplements in Review Says
- Vitamin D 2000 – 5000 IU daily for immunity as vitamin D3.
We recommend vitamin D for immunity if you suspect low levels. The bottom line is that vitamin D is needed for optimal immune function, but many people living in the mid-latitudes are deficient. If you think you may have low levels, then supplemental vitamin D can be a great way to boost your immunity.
Vitamin D3 seems to be slightly superior to D2. Doses between 2000 and 5000 IU of vitamin D3 should be sufficient.
Leave a Reply